
Born with cystic fibrosis (CF), a lung-destroying disease that, according to Cystic Fibrosis Canada, is the country’s most common fatal genetic disease among children and young adults, Pangman had no choice. It was “do or die,” she says. That was in 2008. Unfortunately her body eventually rejected those lungs and, in 2013 she had to do it all over again.
On the phone from Las Vegas, where she and her husband, musician "Colonel" Tom Parker, were taking a vacation before the Junos, Pangman spoke with Samaritanmag about the challenges of being a vocalist when every breath is a little miracle in itself, and of how everyday people can become heroes by giving the Gift of Life. National Organ and Tissue Awareness Week in Canada is April 18-25.
First of all, congratulations on your nomination.
Thank you very much.
I mainly want to talk to you about organ donorship and how you get the word out about that. This is the second time around for you. How different was the second transplant experience from the first?
It was similar but different because every transplant is different. I was a lot more scared the second time because I knew how much hard work it is and how painful it is. I had a little more jitters the second time around. Plus, with rejection, it felt much different. It was just a lot harder to breathe having had rejection, rather than having had CF lungs. Surgery was much longer the second time because they have to remove all the stitches where they’d sown in the first transplant. It was a bit of a bigger production but it’s still amazing to me that you can put a human being through this, and it all went really well, and within two or three weeks they’re home. That right there is sort of mind blowing.
Did you know that this kind of surgery was pioneered in Ontario?
No, not until I was first listed back in 2008. It’s really not been that long since it’s been done.
To think they only did the first lung transplant back in 1983.
I know, but still I have to think about Mary Shelley and Frankenstein and cobbling a body back together and putting the energy through it and… (fake screaming) Ahhhhh! So, 1983 — it took them a long time to get there after Mary Shelley, really. (laughs)
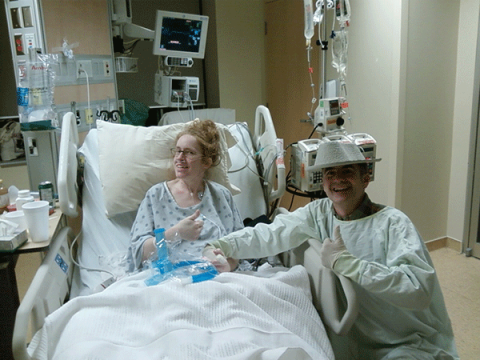
I waited about the same time, which was about six months. It was different. The first time around you’re always in a situation where it’s do or die. You’ve got to do this thing, right? It might have been only, quote “only,” six months but, look, every day feels so much longer because, like, having to shower is exhausting. “What did you do today?” “I had a shower.” ‘Cause [it takes] an oxygen tank, and an attendant and you get out of breath just drying yourself off. Look, every day: walking up stairs, changing your clothes, all of it is totally exhausting, seven days a week. So you do the math: it’s a long time. And you try to keep yourself upbeat. That’s why listening to a lot of music was really helpful to me, really cathartic to me, especially music from the 1930s because it got us through the Great Depression, and then the war years. Those songs are just naturally uplifting. But getting through it is a challenge.
Is listening to music or making music more important to you?
When I was waiting, or now?
Now.
Right now my focus is shifted a little bit towards the creation of music because I’m able to do that again. But I do think that we have to know our roots and where we come from in order to go forward and in order to honour a North American art form. So I always have, for lack of a better term, “vintage” music on my record player. But what excites me right now is picking those inspirations and making them come alive again with the band.
I know that you wrote one song on the latest album. How much original music have you recorded on the others?
There were about five songs on the previous record and there’s usually at least one on a record, but it’s mostly Tin Pan Alley music.
Has your health interfered with your ability to write music yourself?
No. No, in fact having better health has made it easier. Then I can devote time and energy to being creative rather than filling up oxygen tanks and coughing. Just in the act of singing, I can perform better. I can write longer lines. I can sing longer lines ‘cause I’ve got more air power, right? More litres of air to support my ideas, which has truly been a gift to me. We call this the “Gift of Life.” That’s what Ontario’s Trillium Gift of Life Network [TGLF] calls it. Because it is: and you can do the things you love to do, be it write music, be it sing music, be it rock climbing – I don’t rock climb (laughs) – it’s so you can get back to your life.
When your first transplant started going south on you, how long was it before you weren’t able to perform anymore?
As long as I was sitting down, and this is the curious thing: the first transplant I did give up singing about eight weeks before the transplant came because I just was too sick with CF. With CF you’re coughing all the time. With rejection, I wasn’t coughing so I was able to sing practically right up to the end. And when I say “sing,” I mean sitting down, I mean having a phrase that might last 10 seconds cut up into, like, four seconds, then four seconds, then two seconds, taking little breaths in between — so, cheating. But it’s jazz, so I could phrase as I wanted, or phrase as I had available air. We played Massey Hall; we opened for Willie Nelson, and that was six weeks before my call came. So really I sang right up to the end. It was because I didn’t cough when I had rejection.

Yeah, the reason I had the first transplant was because I have this funky genetic code that was in my lungs that was always filling them up with gross stuff that you need to cough up and it scars your lungs. So when I got the transplant in 2008, I essentially ditched that DNA and I didn’t have the cystic fibrosis lungs anymore. What I had was a set of lungs that I had borrowed from somebody that eventually my body rejected, which is the number one fear and the number one risk of transplants. So, with the second transplant it was just a diminishing lung function as my body slowly… chilled the lung (she nervously giggles), which is a pretty claustrophobic feeling. And everybody always says, “Relax. Breathe.” No, it’s the breathing that’s giving me [the problem].
It’s been a couple of years now since the second operation. How does it feel compared to two years after the first one?
I’ve had much less problems the second time, which isn’t to say that problems won’t arise. The first two years after the first transplant were a little bit rocky. There was a lot of infections and problems arising, but this time wasn’t that way. (She sings) “Lungs are better, the second time around.” (laughs) I’m in Vegas, so I had to sing a Sinatra song.
What do you do to get the word out about lung transplants and organ donations? Do you feel that’s a new calling, something that you always do?
For sure a lot of people after having transplants have this desire to tell people about the miracles that this act of altruism can do. A lot of people that have had a transplant wave the flag and I’m not unique in that. What I’m unique in is that I use my donor lungs to make music. So what I usually do is sing to the people for about half an hour, and then I tell them my story so it has some impact, then I close the set out. And that way I’ve introduced to them my voice, then I tell them about my lungs — about the engine behind the voice — and hope that it touches them enough when I’ve finished my set that they really will consider becoming a hero, consider out-living themselves, consider giving the gift of life.
It really is simple. There’s a website called LiveOn.ca and there’s a province-by-province area that you click on to find out where you go to become an organ donor and give your consent. So I encourage people to just do that because we recycle our pop cans and our newspapers and you cannot take your lungs with you when you go. I got lungs, somebody else got a pancreas, kidney, eye, liver. You can save up to eight lives and countless more with tissue donations. So it is something in us that we can do. A friend of mine, he’s about my age, and he got his lung from a man who was 78 years old, so you’re never too old. If you visit that website and you talk to your family about your wishes you can really make a huge, huge difference.
Are there any other organizations or websites you’d like to share?
I would say that for Ontarions, visit BeADonor.ca [managed by TGLF]. That’s the one for Ontario (LiveOn.ca is for Canada-wide information). Just consider becoming a hero and talk to your family about your wishes, in a nutshell.
Is there a community of people who have received lung transplants that communicates with each other and commiserates?
Yeah, well it’s funny because… it’s not funny but it is a community and it is almost like a university where you have your little group and you have your appointments and you sit down and visit and commiserate, like you say. It is a unique thing and probably about a hundred people in Toronto on average get a transplant every year nowadays. Toronto General Hospital has a really active and really successful transplant program, so there’s a lot of us. But we’re still unique amongst the population in that we are breathing with a set of new lungs. They have transplant Olympics; they have transplant groups. It is a bonding experience to go through with your friends. You grieve with them and you celebrate with them and you feel close.
Have you ever met any other singers in the same situation?
I’ve not. Well, there are lots of people, obviously, who like to sing who I’ve not met, but we are internet friends. There’s a woman by the name of Charity Tilleman-Dick and she’s done a bunch of TED Talks about lung transplants. She’s an opera singer. We’ve talked about maybe doing a jazz-meets-opera kinda thing. She is American, so I’m the only one in Canada that I know of. However, Rob Bowman, who is a [music] professor at York University, he’s also a double lung transplant recipient, and he’s a great advocate as well.
How different was your concern about regaining your voice after the second operation, compared to the first?
Well, like I say, it was do or die so I had to do it. But I didn’t worry about it. In fact, both times when they were putting me under I reminded them that I’d like to sing again one day and (in pleading voice), “Please can you be careful when you’re putting the tube down my throat.” But, I mean, when you’re struggling just to survive – when you’re ill you become your illness. I had become my illness and I was no longer out saying I was a singer but I kept my eye on that prize, and yeah, maybe in the back of my mind I worried about it. The first time I had to get used to all the transplant medications so it was a lot more traumatic.
Did you get back to work faster the second time?
I got back to work stupid fast. Stupid fast. It always takes you by surprise when your pager goes off, right? “Oops! I’ve booked the guys, booked the gigs…” One of them was the Port Hope All-Canadian Jazz Festival, but I didn’t know when my transplant was going to come along then. They knew, just as Massey Hall had known, what was coming down the pipe for me. I remember (she laughs) lying in my hospital bed and going in my iPhone and trying all my subs: “Can you do this gig in Port Hope?” And nobody could do the gig in Port Hope, which I think was five weeks after the surgery. Or was it four weeks [she asks her husband, who is in the room with her]? I’ll have to check it. Anyways, I still couldn’t wear a bra because of the incisions, and I sang the gig, which was crazy. I didn’t know if I could sing; I didn’t know what would happen when I opened my mouth, but it was an awesome moment because it was the first time that I got to sing with my present lungs and did it in front of a beautiful crowd with my very good friends in my band. And we got a standing ovation.
I don’t know if this is an awful question or not, but I’ve read that the typical lifespan for transplanted lungs is three to five years. Is this something that you’ll have to go through at least a couple more times?
They have not done a third double lung transplant, at least not in Canada, so (she pauses) they’re not cheaper by the dozen. Yeah, the statistics are kinda scary which is why (she sighs)… I try and seize the day. But I think everybody should. You just don’t know when the anvil is going to fall and that’s not to say that’s why you go on vacation to Nevada, but life is precious. Life is fine and I’m in a spot where I enjoy myself, I love what I do. I love singing and I love bringing music to people and I just try and put those statistics out of my mind.
Nike Air Max 200