Pekar suffers from Polycystic Kidney Disease (PKD). Though rarely name-checked in the evil pantheon of life-threatening genetic diseases, PKD is nevertheless maddeningly common, affecting more people than Down syndrome, cystic fibrosis, muscular dystrophy, hemophilia and sickle cell anemia combined, according to the PKD Foundation of Canada.
Pekar was diagnosed in 1979, when she developed a kidney stone after delivering her first son, Arie, the year before. Arie also developed PKD. “At the time my doctor told me not to worry about it and many years passed before I really understood what having PKD meant,” Pekar tells Samaritanmag.
“GPs [general practitioners] back then just didn’t know much about something like this so I was not put in the care of a nephrologist [kidney doctor] and not told that it was hereditary or that I could pass this down to my children. By the time I had my second son in 1982 and got very sick with another kidney stone, I was finally put under the case of a nephrologist.”
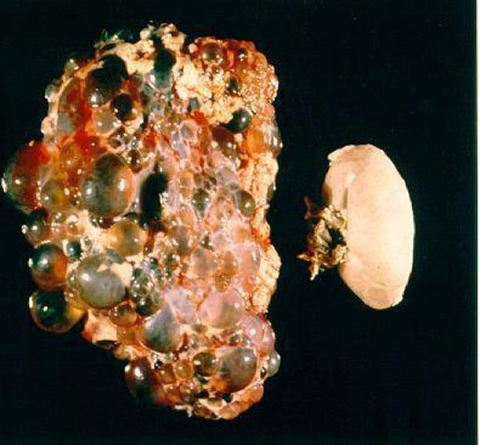
Even among genetic diseases, PKD is especially nefarious. According to the PKD Foundation of Canada, over time, cysts develop on the kidneys, then grow and multiply, causing the kidney to increase sometimes dramatically in size.
Although a normal kidney is roughly the size of a human fist, PKD kidneys can grow to be the size of a football or larger and weigh as much as 38 pounds. Other organs, such as the pancreas and liver, also can be affected by PKD cysts.
Some 12.5 million newborns, children and adults worldwide — 66,000 of them in Canada or roughly 1 in 500 for the dominant form of PKD and 1-in-20,000 for the recessive form — battle the disease, according to the PKD Foundation. About 50 percent of people with PKD will develop kidney failure by the age of 50 and be forced to depend on dialysis or a transplant to live. There is no cure.
The Burlington, Ont.-based Pekar, who has endured two failed kidney transplants — and has been on dialysis nearly 20 years — is awaiting a third. Son Arie is also desperate for a life-saving new kidney. Younger brother Joshua avoided the nasty genetic fate of his older brother and mother, but has been deemed unsuitable for a kidney donation. So the interminable wait goes on.
Though the whole notion of organ donation is a private matter, Pekar says she is going public now, during National Kidney Month which falls each March, because the search for a kidney for herself and her son has reached critical proportions.
“My blood type is A negative and I need a donor because I am coming to the end of the road,” she laughs wryly. “I’ve been on dialysis longer than anticipated; most people don’t live this long. My son Arie just turned 35. So I am hoping for transplant number three and another one for him. That’s my story. So going public is what we’re doing.”

“Unfortunately, the Canadian registration rate is difficult to determine because not all provinces actually have a registry,” she adds. “In Ontario, you can register online at www.BeADonor.ca. It’s important to note that a signed donor card is no longer enough. You must register.”
The enormous potential benefit from organ donation should motivate us all. A single organ donor can save up to eight lives through the donation of heart, lungs (two), liver, kidneys (two), pancreas and small bowel.
“And up to 75 additional lives can be enhanced through the gift of tissue, which includes corneas, heart valves, bone and skin,” adds Hollingsworth.
Pekar agrees that organ donation — recently in the spotlight via Ottawa-based double-lung transplant recipient and Ellen De Generes favourite Hélène Campbell — must land on people’s radar. Her second kidney transplant in the mid-1990s was harvested from a cadaver donor who gave consent (or his/her family did); her first came from her now-ex-husband around 1992.
“In both cases I never got off dialysis and they only lasted about two weeks. They just never took.” These days, she is on dialysis six days a week. “I try and look at it like walking a dog. I try and get it over and done with and then, depending on how I feel afterwards, I get on with my day.”
Jeff Robertson also knows a thing or two about PKD and not just because he has served as executive director of the PKD Foundation of Canada for four years. “My parents founded it on a provincial level in 1994. We became a national organization in 2009,” he says.
“Both my mother and my grandmother are affected by PKD,” Roberston explains, adding that he and his sister dodged the bullet. “And it doesn’t skip a generation which means we won’t pass it along to our children when the time comes.
“So our family is a good example of the lack of consistency with respect to this disease. My grandmother Myrn Millen is 89-years-old and only in the last few years she’s been experiencing hypertension, which is pretty amazing given her age. My mother Jan Roberston, who is 59, has had two life-saving liver transplants and she is going to need a kidney transplant in the next five to eight years.
“National Kidney Month allows us to bring this to people’s attention and also, to encourage people to live a kidney-conscious lifestyle — drink lots of water, cut back on sodium and caffeine, monitor the level of protein you ingest.
“We want to make sure people understand what chronic kidney disease is, what PKD is and how important organ donation is to our organization,” Robertson says. “I can’t begin to describe the incredible transformative impact those liver transplants had on mother. This issue is so important.”
Patike